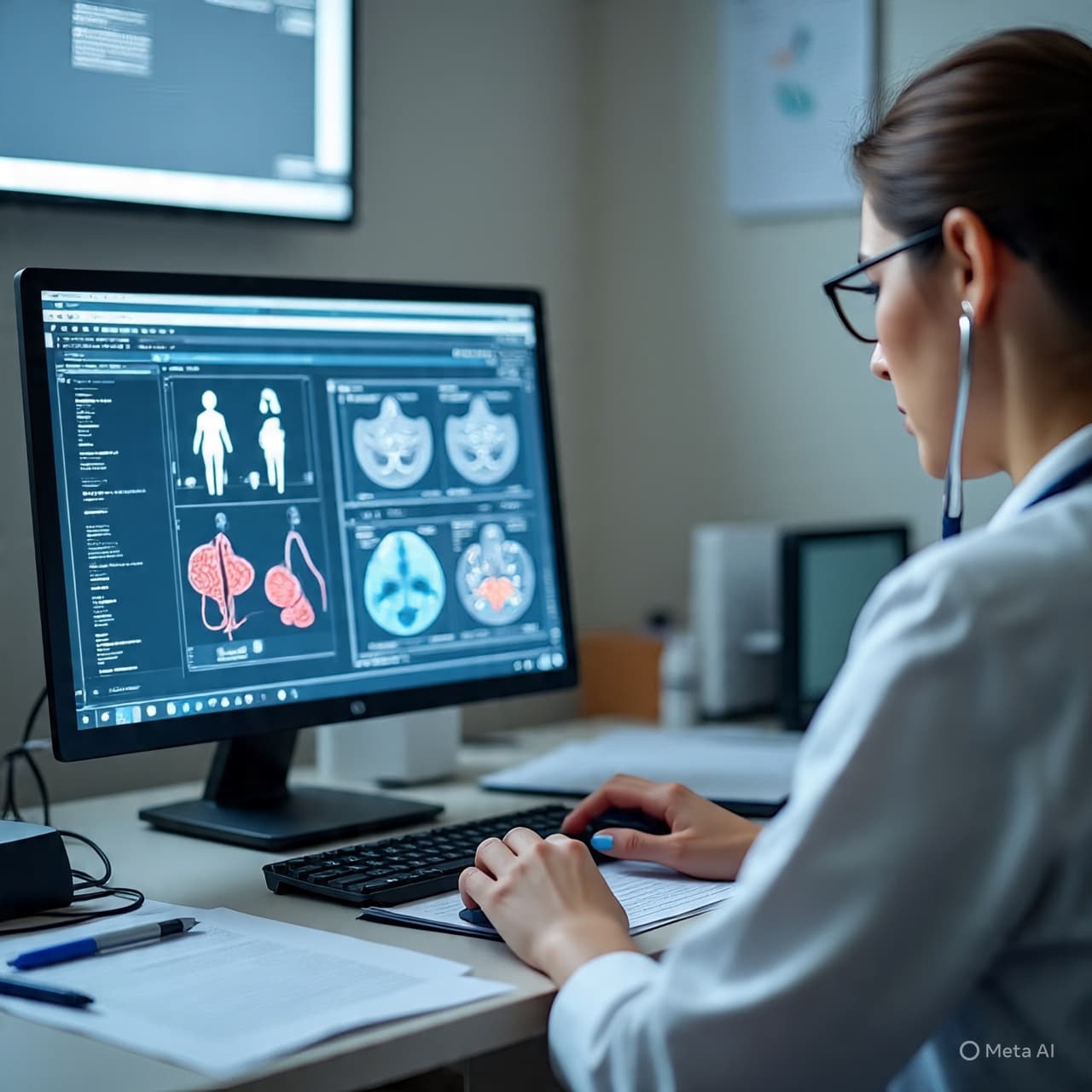
In hospitals around the world, childhood cancer wards often carry a quiet rhythm. There are the small rituals of daily care—nurses adjusting IV lines, parents reading bedtime stories beside hospital beds, doctors studying charts beneath the glow of computer screens. In these spaces, medicine is both intensely technical and deeply human.
And increasingly, another presence is joining the room.
Artificial intelligence has begun to weave its way into modern medicine, offering tools that can scan medical images, interpret genetic data, and help doctors detect patterns that might otherwise remain hidden. In fields such as oncology, where timing and precision can shape outcomes, the promise of these tools has drawn particular attention.
But when the patients are children, the conversation around technology becomes something more than efficiency or accuracy. It becomes a question of responsibility.
Some researchers now describe pediatric cancer care as a kind of “stress test” for artificial intelligence—an environment where the true strengths and limits of medical algorithms are revealed.
Childhood cancers differ in many ways from those that affect adults. They are often rarer, biologically distinct, and sometimes more complex to diagnose. Because of this rarity, the amount of available medical data can be smaller, making it more challenging to train AI systems that rely on large datasets.
Yet it is precisely in these complicated spaces that AI tools are beginning to show potential.
Researchers have developed systems capable of analyzing pathology slides, identifying subtle patterns in tumor cells that may help classify cancers more quickly. Other tools examine medical imaging—such as MRI or CT scans—to detect changes that might be difficult for the human eye to recognize in early stages.
In genomic medicine, artificial intelligence is also helping scientists interpret enormous sets of genetic information, searching for mutations that could guide personalized treatments for young patients.
These developments can feel quietly remarkable. What once required weeks of analysis may sometimes be narrowed to hours or days with the assistance of machine learning systems.
Still, the presence of AI in pediatric oncology raises a different set of questions alongside the technological excitement.
Children, after all, cannot advocate for themselves in the same way adults can. Their care involves families, clinicians, and institutions working together to make decisions that may shape a lifetime.
For that reason, many experts argue that pediatric medicine demands an especially careful approach to emerging technologies.
Algorithms must be transparent enough for clinicians to understand how conclusions are reached. Data used to train these systems must be diverse and carefully governed to avoid hidden biases. And perhaps most importantly, AI must remain a tool that supports physicians rather than replacing the human judgment that lies at the center of medical care.
Some researchers suggest that pediatric oncology offers a uniquely revealing lens for evaluating whether AI systems truly work in real clinical settings.
If a technology can operate safely and effectively in a field defined by rare diseases, complex decisions, and vulnerable patients, it may offer lessons that extend far beyond childhood cancer wards.
The testing ground, in other words, is not only technical but ethical.
Doctors must learn how to integrate algorithmic insights into conversations with families. Researchers must determine how data can be shared internationally to improve systems while protecting privacy. Hospitals must decide how much trust to place in tools that continue to evolve.
These are not questions that can be solved by software alone.
They require dialogue among clinicians, engineers, ethicists, and patients’ families—people whose experiences often differ but whose goals converge on the same outcome: better care for children.
For many experts, that shared purpose is what ultimately defines “good” technology in medicine.
It is not merely about speed or efficiency, nor about the novelty of advanced algorithms. It is about whether the tools created by science genuinely serve the people who depend on them most.
In pediatric oncology, where the stakes are measured in young lives and long futures, that test becomes especially clear.
Artificial intelligence may continue to grow more capable in the years ahead. But within the quiet halls of children’s hospitals, the most important measure may remain unchanged.
Technology must prove not only that it works, but that it cares.
AI Image Disclaimer Images in this article are AI-generated illustrations, meant for concept only.
Sources Nature Medicine STAT News The New York Times MIT Technology Review The Lancet Digital Health